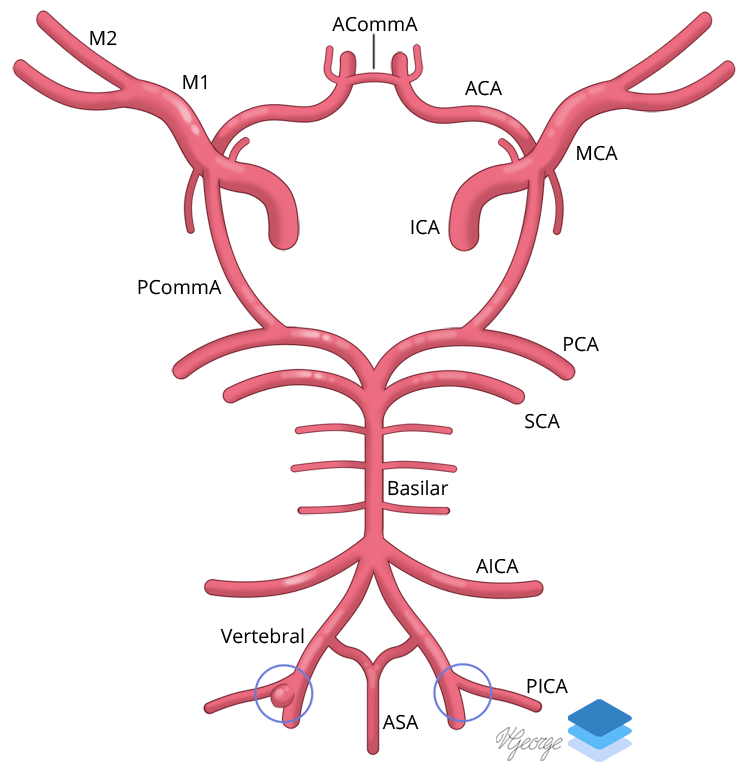
A reflux arc involving phrenic, vagal, and central midbrain modulation is likely responsible for hiccups. Hiccups are defined as sudden-onset involuntary contractions of the diaphragm followed by immediate inspiration and laryngeal closure, and they are considered intractable if prolonged beyond 1 month. Sindou M, Keravel Y (2009) Traitement neurochirurgical de la névralgie vago-glossopharyngienne. Wang J, Yu R, Qu C, Jiang J, Wang C, Meng Q, Wei S (2018) Does glossopharyngeal neuralgia need rhizotomy in neurovascular decompression surgery? J Craniofac Surg. Ann Indian Acad Neurol 16(1):1–8 (Available at: ) Singh P, Kaur M, Trikha A (2013) An uncommonly common: glossopharyngeal neuralgia. Headache Classification Committee of the International Headache Society (IHS) (2018) The International Classification of Headache Disorders. Pearce J (2006) Glossopharyngeal Neuralgia. The Author(s), under exclusive licence to Springer-Verlag GmbH Germany, part of Springer Nature. Although SRS may be a viable alternative treatment for GPN, further studies must be done to evaluate long-term treatment efficacy.Ĭranial nerves Glossopharyngeal nerve disease Microvascular decompression surgery Nerve compression syndromes Radiosurgery Treatment outcomes. Patients with MVD alone presented with less adverse effects than the group that underwent MVD plus rhizotomy. MVD, rhizotomy, and SRS are effective methods to treat GPN as they help achieve instant pain relief and the decrease use of medication. SRS had promising results in pain reduction when using 75 Gy radiation or higher however, long-term rates of pain relief were lower. The most common adverse effects observed after a rhizotomy were dysphagia and dysesthesia along the distribution of the glossopharyngeal nerve. Rhizotomy alone shows an instant pain relief in 85-100% of the patients, but rate of long-term pain relief was lower compared to MVD. The most common complication found on MVD surgery was found to be transient hoarseness and transient dysphagia. MVD alone was successful achieving pain relief immediately postoperatively in about 85% of patients, and also long term in 65-90% of patients. Of all included patients with glossopharyngeal neuralgia, the most common offending artery compressing the glossopharyngeal nerve was the posterior inferior cerebellar artery (PICA). A total of 36 articles were included for review. We consulted PubMed and Medline, including articles from the year 2000 onwards. We included retrospective studies and case reports in our search. Moreover, we sought to explore if SRS, a minimally invasive alternative surgical option, achieves comparable outcomes. We conducted a systematic review to analyze whether MVD without rhizotomy is an equally effective treatment for GPN as MVD with the use of concurrent rhizotomy. More recently, the use of stereotactic radiosurgery (SRS) has been utilized as an alternative treatment method to relieve patient symptoms by causing nerve ablation. Pharmacological treatment with anticonvulsants is the first line of treatment however, about 25% of patients remain symptomatic and require surgical intervention, which is usually done via microvascular decompression (MVD) with or without rhizotomy. Glossopharyngeal neuralgia (GPN) is a neurological condition characterized by paroxysmal, stabbing-like pain along the distribution of the glossopharyngeal nerve that lasts from a couple of seconds to minutes.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
